Background
Peripheral Artery Disease (PAD) is atherosclerotic artery disease, most typically in a lower extremity. PAD Guideline Directed Medical Therapy (GDMT) is used in only 30-40% of cases due to clinical knowledge gaps. There is significant evidence that adherence to 4 recommended therapies reduces risk of adverse cardiovascular (36%) and limb events (44%).
Only 10% of patients with PAD exhibit classic claudication.
- Approximately 50% are asymptomatic
- Approximately 40% have atypical leg symptoms (i.e. knee pain, hip pain, etc.)
African Americans have twice the risk compared with other races.
High annual mortality of 5-7% in PAD patients without critical limb ischemia.
Diagnosis
Risk Factors
- Age > 65
- Tobacco use
- Diabetes, hypertension, hyperlipidemia, AAA, known atherosclerotic disease
- Family history of PAD
History Clues
- Lower extremity pain, more specifically claudication
- Other non-joint related exertional leg symptoms
- Impaired walking
Claudication is reproducible discomfort (cramping, aching, pain) or fatigue in the muscles of the lower extremity occurring with exertion and relieved within 10 minutes of rest.
Physical Exam
- Diminished pulses
- Vascular bruits
- Pallor
- Rubor
- Non-healing wounds
- Any evidence of lower extremity gangrene
Differential diagnosis may be broad and includes
Venous ulcer, symptomatic Baker’s cyst, local trauma, neuropathy, infection, small artery occlusion (microangiopathy), drug reaction/ toxicity, autoimmune injury, inflammatory disorder, spinal stenosis, nerve root compression, arthritis of hip, ankle or foot, chronic compartment syndrome
Testing and Assessment for Intervention
| Test | Indication | Next steps | |
|---|---|---|---|
| Ankle Brachial Index (ABI) | If history and/or exam are suggestive of PAD Screening is reasonable if patient is asymptomatic but presents with PAD risk factors |
ABI 1.0-1.39 | Look for other causes of symptoms/abnormal exam |
| ABI 0.91-0.99 | Possible PAD → Obtain Exercise Treadmill ABI or 6 minute walking test | ||
| ABI < 0.90 | If no critical limb ischiemia, begin guideline-directed medical therapy | ||
| ABI > 1.40 | Obtain Toe Brachial Index (TBI) TBI < 0.70 indicates PAD |
||
| If CLI suspected and ABI non-compressible, obtain TBI with waveforms or toe perfusion pressure | |||
| CTA or MRA | If considering revascularization procedure or surgery | Consider revascularization for acute limb ischemia (ALI), critical leg ischemia (CLI), symptomatic iliac disease, or infrainguinal disease that significantly impairs functional status/QoL despite GDMT and exercise therapy | |
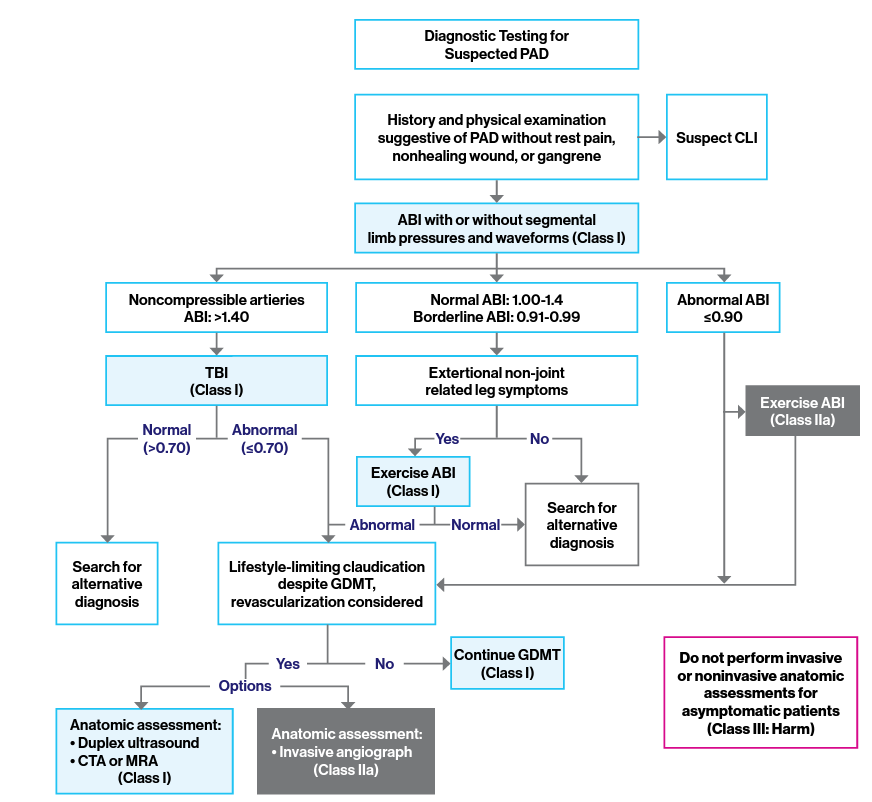

Management and Treatment
Goals
- Eliminate/reduce claudication to improve mobility, functional status, and health-related QoL
- Reduce risk of fatal and non-fatal ischemic cardiovascular events and limb loss
PAD Management Checklist
| Intervention | Frequency/ Dosing | Considerations | |
|---|---|---|---|
| Prior to any vascular intervention | Asymptomatic PAD (ABI < 0.9): ASA or Clopidogrel | ASA 81mg qd or Plavix 75 mg qd | |
| Symptomatic PAD: ASA + Rivaroxaban | ASA 81 mg Rivaroxaban 2.5 mg bid | ASA and Rivaroxaban may improve CV outcomes, with modestly increased risk of bleeding Dual antiplatelet therapy (DAPT) generally not recommended for symptomatic or asymptomatic PAD |
|
| Symptomatic PAD AND increased risk of bleeding: ASA OR Clopidogrel | Aspirin 81 mg qd OR Clopidogrel 75 mg qd | ||
| Post-vascular intervention | ASA + Rivaroxaban OR ASA + Clopidogrel | ASA 81 mg qd + Rivaroxaban 2.5 mg bid OR ASA 81 mg qd + Clopidogrel 75 mg qd | ASA and Rivaroxaban may reduce risk of adverse CV and limb events after revascularization If risk of bleeding is increased, DAPT with ASA and Clopidogrel may be used |
| Claudication and walking | Initiate Cilostazol | 100 mg bid | Side effects: headache, palpitations, and diarrhea ! Contraindicated in presence of heart failure and/or EF <40% |
| Hypertension management | BP <130/80 | Measure monthly until at goal; every 3-6 months thereafter | No preferred agent in absence of other disorders (DM, CKD, CHF) Beta-blockers are not associated with worsening claudication First line is often ACE inhibitors |
| Diabetes management | HbA1c <7% | Measure every 3 months until at goal; every 6 months thereafter | Intensify medications to optimize control Biannual foot exam with monofilament test |
| Lipid management | LDL target <70 mg/dl | Ongoing monitoring | Moderate or high intensity statin therapy, indicated for all PAD patients, regardless of cholesterol level, to reach LDL target Ezetimibe ($) may be added to achieve LDL goal PCSK-9 inhibitors ($$$) may reduce CV and adverse limb events when added to statins, though expensive |
| Tobacco cessation | Annual screening and follow up for all patients, refer to smoking cessation program, medication if appropriate | Address at every visit for active smokers | Provide a medication prescription (bupropion, varenicline, or nicotine replacement) even if patient not ready to fill, so the patient does not have to wait once ready Detailed discussion on “what will happen to your health and limbs if you continue smoking" |
| Exercise program | Supervised or home-based (guidelines) | 3-5 sessions per week | Home exercise 3-5x/week: begin with 10 minutes of walking exercise per session; increase walking by 5 min per session per week, until patient is walking 45-50 min per session (excluding rest periods) Treadmill-based program: 30-60 minute exercise sessions, 3x/week, for minimum of 12 weeks, with additional 36 sessions, if warranted |
| Revascularization | Claudication severity, presence of iliac disease, and QoL drives revascularization decision | Perform in conjunction with GDMT and exercise therapy | Iliac disease is generally treated with revascularization Below Iliac disease: generally, GDMT + exercise are initial therapies When CLI present, endovascular and/or surgical procedures used to provide in-line blood flow to 1 patent artery Surgical patency rates higher than endovascular procedures, but with more complications Post-procedure follow-up with periodic ABI measurements and, in some patients, Doppler ultrasound is warranted |
Additional Management Considerations
Supervised/Home Exercise Programs
- Effectively reduce claudication and atypical symptoms, improve both functioning and QoL, alone or in conjunction with revascularization
- Other exercise strategies include upper-body ergometry and cycling for patients with leg amputations
Foot care for patients with diabetes
- Biannual foot exams including pulses/perfusion; use 10g monofilament and either temp, pinprick, vibration, or ankle reflexes to detect neuropathy
- Refer patients with PAD to podiatrist
- If foot ulcer present, refer to vascular specialist
Minimizing Risk of Tissue Loss
- Prevention: patient education regarding healthy foot behaviors (e.g., daily feet inspection; foot care and hygiene, including safe toenail cutting strategies; avoidance of barefoot walking, proper shoes)
- Prompt diagnosis and treatment of infections and other foot disorders
- Suspect if patient has local pain, tenderness, inflammatory reaction around wound, pretibial edema, discharge or odor, or signs of a systemic inflammatory response
- Treatment of deep soft-tissue infections typically requires prompt surgical drainage, vascular imaging, and timely revascularization
- Goal: complete wound healing
Acute Limb Ischemia
ALI is a medical emergency typically requiring prompt anticoagulation, emergency consultation with vascular specialist, and thrombolysis or thrombectomy for viable limbs.
When to Refer
Consider referring the patient to specialty care in the below cases:
Vascular Specialist
- Debilitating claudication
- Lifestyle limiting activity
- Diabetes and foot wound
- Non-healing foot wounds
- Known PAD and foot wound
Vascular Medicine/Cardiology
- Assistance in managing coexisting PAD risk factors, such as hypertension, lipid disorders
- Pre-operative assessment of high-risk patients
- Confirm diagnosis of PAD when symptoms are atypical and/or normal/ borderline noninvasive tests
- Call 212-241-9454 to request an appointment with Dr. Olin at The Lauder Family Cardiovascular Ambulatory Center
Vascular Surgery
- Determine the most appropriate diagnostic testing and arrange
- Revascularization in patients with refractory symptoms despite GDMT
- Manage acute and critical limb ischemia
- Treatment of non-healing skin and soft tissue infections and non-healing wounds
Diagnostic Testing
All Locations
- ABI Testing
- Exercise ABI
- Toe Brachial Index (with waveforms)
- Toe Perfusion Pressure
MS-West & MS Downtown Only
- Transcutaneous 02 pressure
| Hospital | Address | Phone |
|---|---|---|
| The Mount Sinai Hospital | 17 East 102nd Street, 4th Floor, New York, NY 10029 | 212-659-8554 |
| 1190 Fifth Avenue, 1st Floor GP-1 Center, New York, NY 10029 | 212-241-5315 | |
| Mount Sinai Morningside | 440 West 114th Street, Ambulatory Care Center, New York, NY 10025 CVI 2nd Floor Suite 220 or ACC 1 – 1st Floor | 212-523-3360 |
| Mount Sinai West | 425 West 59th Street, 7th Floor, New York, NY 10019 | 212-523-4797 |
| Mount Sinai Queens | Mount Sinai Queens Pavilion 25-20 30th Avenue, 5th Floor, Astoria, NY 11102 | 718-808-7777 |
| Mount Sinai Downtown | 10 Union Square East, 2nd Floor Suite 2N, New York, NY 10003 | 212-844-5559 |
| Mount Sinai Brooklyn | MS Outpatient Vascular Office: 3131 Kings Hwy Room LL07 | 718-677-0109 |
| Mount Sinai South Nassau | 1420 Broadway 2nd Floor, Hewlett, NY 11557 | 516-374-8682 Wound Care: 516-764-4325 |
Note: Wound care is offered at all locations, except MS-South Nassau sees patients at their Wound Care Center
Interventional Radiology
- Diagnostic angiography and therapeutic catheter-based interventions in symptomatic PAD
| Hospital | Address | Phone |
|---|---|---|
| Mount Sinai West | 1000 Tenth Avenue 2nd Floor New York, NY 10019 | 212-241-4046 (Press 1) |
| Mount Sinai East | 5 East 98th Street 12th Floor New York, NY 10029 | 212-241-4046 (Press 1) |
| Mount Sinai Queens | 25-10 30th Avenue, Astoria, NY 11102 | 347-408-8234 |
Click here for additional locations
Supervised Office-Based Exercise Program
- Cardiac Rehabilitation at the Mount Sinai Hospital (212-427-1540)
- Physical Therapy at Mount Sinai Downtown Union Square (Use Epic PT referral or call 212-844-8750)
Team-Based Care
Leverage the support of additional care team members to effective manage patients with chronic conditions. Available services include:
- Clinical pharmacists
- Certified Diabetes Educators (CDE/Wellness Coaches)
- Care management
- Behavioral health
Home Health Care Referral
Home-based care may be arranged using “Consult to Visiting Nurse Services” order in Epic for wound care, physical therapy, nursing education and visits, and more.
Next Steps
- Print and share resources with your patients to empower them to meet their care goals
- Check out PAD Condition Management Tips for quick takeaways to keep you up-to-date on management guidelines
